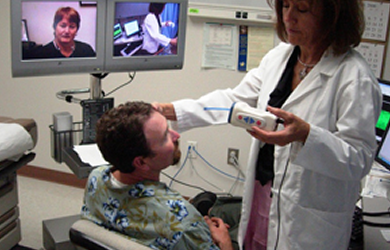
He had never been to an appointment like this.
Veteran Richard Martinez sat in the exam room while his nurse practitioner, Carla Uran, listened to his heart and lungs and took his blood pressure.
After conducting an EKG (electrocardiogram) to check for heart irregularities, the two discussed Martinez’s health. There was one distinctive factor that made this appointment different: Martinez and Uran were 120 miles apart.
Clinical Video Telehealth (CVT) gives patients and providers the opportunity to conduct several aspects of medical examinations that do not require in-person visits. Veterans are able to visit a VA clinic near their home, connect to medical centers through videoconferencing, and transfer medical information by way of specially-designed telecommunications equipment.
Who Wants a Four-Hour Drive? Nobody!

Martinez lives in Pueblo, Colorado, which is more than two hours away from both Alamosa and Denver – the nearest VA locations with in-house doctors and nurse practitioners.
Uran is based in Alamosa but provides care for Veterans in smaller clinics in Pueblo and La Junta (nearly a four-hour drive from her home). She used to spend a significant amount of time on the road in order to serve her patients.
“My commute was working, but my patient load was smaller and I wasn’t as readily available for my patients,” explained Uran. CVT has allowed her to better utilize her time and provide care for more Veterans. Now, neither patient nor provider is required to spend excessive amounts of time on the road.” Telehealth consultations can be just as good as in-person consultations – it depends on the medical reason for the visit,” said Uran. For example, if a patient comes in with a cold, she can have a nurse perform the basic assessment activities on site at the smaller clinic, and have a specialized video camera pointed in the patient’s ear, nose and throat.
Martinez, as a first-time participant of telehealth, described his experience as “different.” He explained, “I thought it was a good idea, especially because I’m not much for long-distance driving.” Although he missed the hands-on experience, he was happy to know he had medical expertise on hand when he needed it – without spending hours on the road.
In several regions across the country, there is not a dense enough Veteran population to justify a fully-staffed medical centers. Telehealth provides access to quality healthcare for Veterans in many rural areas.
“Out in the Boonies”
Bill Morgan is an army Veteran who lives, as he puts it, “out in the boonies” near Craig, Colorado. He loves his rural home, but it means he must drive 160 miles to the nearest VA Medical Center in Grand Junction, Colorado. Morgan requires a blood test once a month, so it is no surprise that he appreciates having access to telehealth through the VA clinic in Craig.
“I love it because it saves me a trip all the way to Grand Junction. Nobody likes that three-hour drive – especially in winter with the icy conditions,” said Morgan. In addition to regular medical check-ups and blood tests, Morgan participates in another telehealth service, MOVE!, a national weight management program.
“Telehealth lends itself to the MOVE! program because it is difficult to find necessary staff to participate in each rural location,” said Jeff Lowe, Special Projects Manager for the Office of Telehealth. Several VA clinics now host MOVE! sessions via videoconferencing to larger medical centers. Other educational programs include diabetic education and smoking cessation.
Morgan has been pleased with all services provided through Craig’s telehealth program. “Telehealth is convenient,the staff takes great care of me, and it saves me a lot of time,” said Morgan.

Teleservices for 17,000 Veterans
CVT primary care is just one of the many ways in which telehealth connects Veterans to healthcare services. The VA provides services in telerehabilitation,teledermatology, telemental health, teleretinal imaging and the list is growing.
Expansion of services is continuously in the works. The VA Rocky Mountain Network alone (spanning Montana, Wyoming,Utah and Colorado) provided telehealth care to 17,000 Veterans last year. The same region is also in the process of opening 10 primary care telehealth clinics equipped with nursing and technical staff ready to connect Veterans to far-reaching practitioners.
Future plans are “to expand the size and scope of telehealth programs to focus on expanding access to care for Veterans in rural locations,” said Dr. Adam Darkins, Chief Consultant of Care Coordination Services at the VA. “This will reduce the need for travel to specialist services, thus increasing the quality and timeliness of care.”
Article Source: Megan Tyson, VA Staff Writer for United Sates Department of Veterans Affairs, January 29, 2010